Cirrhosis of the Liver: What It Is, Symptom & Treatment Explained
Cirrhosis of the liver is a serious condition that can quietly affect your health without obvious signs at first. If you’ve noticed unusual tiredness, stomach discomfort, or changes in your skin, it’s important to understand what might be happening inside your body.
This article will guide you through what cirrhosis really is, how to recognize its symptoms early, and what treatment options can help protect your liver. Knowing these facts could make a big difference for your health—so keep reading to learn how to take control and stay informed.

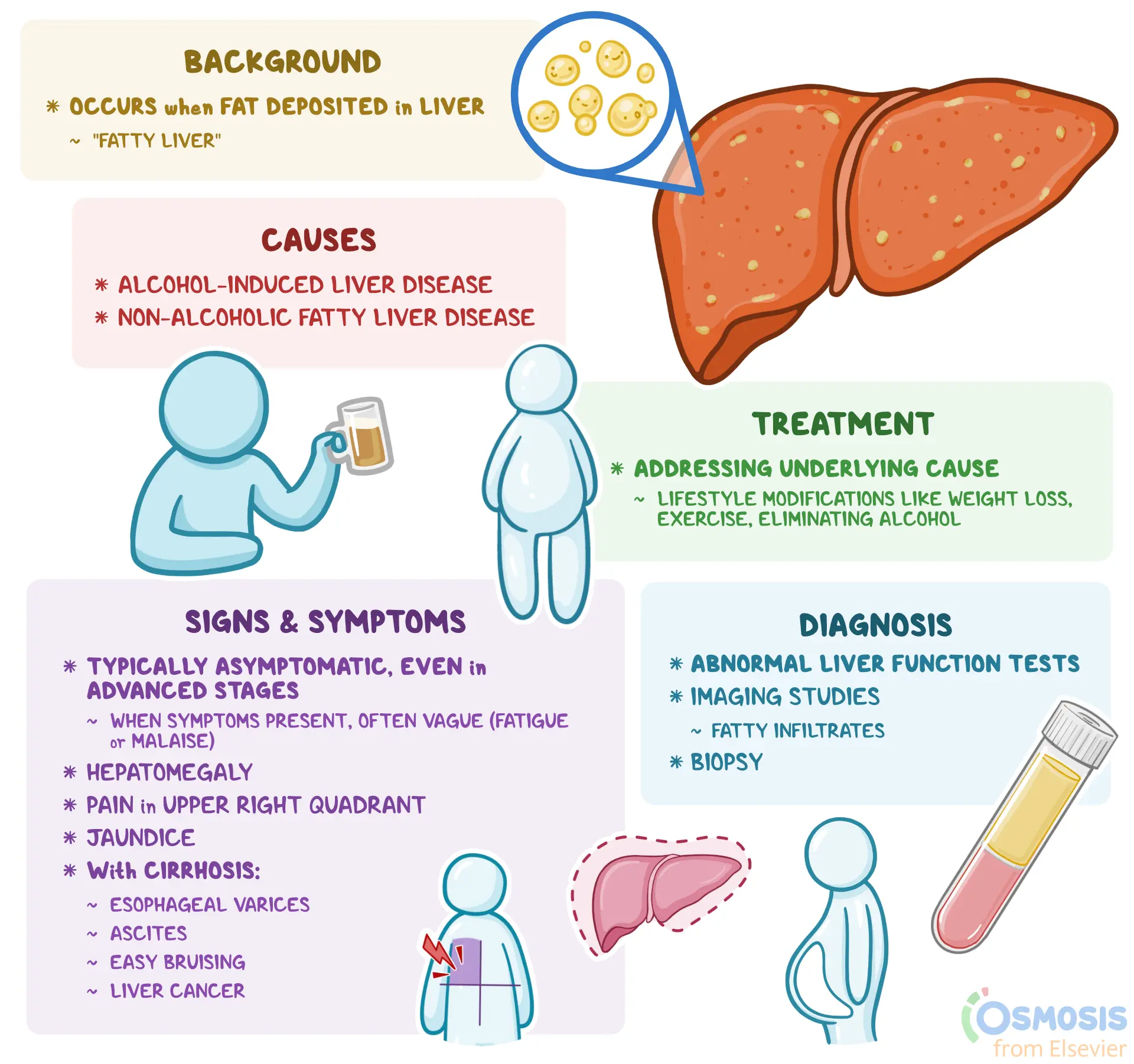
Credit: www.osmosis.org
Causes Of Cirrhosis
Cirrhosis of the liver is a serious condition that affects how the liver works. It happens when healthy liver tissue is replaced by scar tissue. This scarring stops the liver from working well. Many things can cause cirrhosis. Understanding the causes of cirrhosis helps prevent it and guides treatment. The main causes include chronic alcohol use, viral hepatitis, nonalcoholic fatty liver disease, and other factors. Each cause damages the liver in different ways and may require different care.
Chronic Alcohol Use
Chronic alcohol use is one of the most common causes of cirrhosis. Drinking too much alcohol over many years can harm liver cells. The liver tries to repair itself, but constant damage causes scars. These scars block blood flow and reduce liver function.
How alcohol affects the liver:
- Alcohol breaks down into harmful chemicals that injure liver cells.
- Repeated injury causes inflammation and tissue death.
- Scar tissue replaces healthy cells, leading to cirrhosis.
Not everyone who drinks heavily gets cirrhosis. Factors like genetics, diet, and other illnesses play a role. Here is a simple table showing the risk related to alcohol intake:
| Alcohol Intake | Risk of Cirrhosis |
|---|---|
| Less than 20g/day | Low risk |
| 20-40g/day | Moderate risk |
| More than 40g/day | High risk |
Stopping alcohol use early can prevent cirrhosis or slow its progress. Medical help and support groups improve chances of quitting.
Viral Hepatitis
Viral hepatitis is another major cause of cirrhosis. It is an infection that causes liver inflammation. The most common types that lead to cirrhosis are hepatitis B and hepatitis C. Both viruses damage liver cells over time.
How viral hepatitis causes cirrhosis:
- The virus infects liver cells and causes inflammation.
- Ongoing infection leads to cell injury and death.
- The liver forms scar tissue to repair damage.
- Excessive scarring reduces liver function.
Risk factors for viral hepatitis include:
- Sharing needles or personal items
- Unprotected sex
- Blood transfusions before screening
- Mother-to-child transmission during birth
Vaccines exist for hepatitis B but not for hepatitis C. Antiviral treatments can control infections and lower cirrhosis risk. Early diagnosis improves outcomes.
Nonalcoholic Fatty Liver Disease
Nonalcoholic fatty liver disease (NAFLD) happens when fat builds up in the liver without alcohol use. It is common in people with obesity, diabetes, or high cholesterol. NAFLD can progress to a severe form called nonalcoholic steatohepatitis (NASH), which causes inflammation and scarring.
Key points about NAFLD and cirrhosis:
- Fat accumulation stresses liver cells.
- Inflammation damages liver tissue.
- Scar tissue forms, leading to cirrhosis in some cases.
Risk factors for NAFLD include:
| Risk Factor | Description |
|---|---|
| Obesity | Excess body fat increases liver fat. |
| Type 2 Diabetes | High blood sugar harms liver cells. |
| High Cholesterol | Fatty deposits build up in the liver. |
NAFLD is preventable with a healthy diet, exercise, and weight control. Monitoring liver health helps catch problems early.
Other Factors
Several other factors can cause cirrhosis. These are less common but important to know. They include genetic diseases, long-term bile duct problems, and some medicines.
Common other causes of cirrhosis:
- Autoimmune Hepatitis: The immune system attacks the liver.
- Primary Biliary Cholangitis: Damage to bile ducts causes scarring.
- Hemochromatosis: Too much iron builds up in the liver.
- Wilson’s Disease: Copper accumulates abnormally in the liver.
- Medications and Toxins: Long-term use of some drugs or poisons.
Each condition damages the liver differently. Testing and specific treatments are needed. Early diagnosis improves treatment success. Avoiding liver toxins and regular medical checkups help protect the liver.
Signs And Symptoms
Cirrhosis of the liver is a serious condition where healthy liver tissue is replaced by scar tissue. This scar tissue blocks the flow of blood through the liver and slows its ability to process nutrients, hormones, and drugs. Recognizing the signs and symptoms early can help manage the disease better and improve quality of life. Symptoms change as the disease progresses, starting mild and becoming more severe.
Early Symptoms
In the beginning, cirrhosis may not cause obvious symptoms. Many people feel well and do not notice any problems. Early signs are often subtle and easy to miss. These symptoms include:
- Fatigue: Feeling unusually tired or weak.
- Loss of appetite: Reduced desire to eat, leading to weight loss.
- Nausea: Mild stomach discomfort or feeling sick.
- Abdominal discomfort: Slight pain or fullness in the upper right abdomen.
- Itchy skin: Mild itching without rash.
These symptoms occur because the liver starts to lose its ability to filter toxins and produce important proteins. The body reacts to these changes, but the liver still works enough to avoid more serious signs.
| Symptom | Description | Impact |
|---|---|---|
| Fatigue | Low energy and tiredness | Reduced daily activity |
| Loss of appetite | Less interest in food | Weight loss |
| Nausea | Feeling sick to stomach | Discomfort after eating |
| Abdominal discomfort | Mild pain in liver area | Unease or fullness |
| Itchy skin | Unexplained itching sensation | Minor irritation |
Advanced Symptoms
As cirrhosis progresses, symptoms become more obvious and severe. The liver loses more function and scar tissue blocks blood flow. This causes:
- Jaundice: Yellowing of skin and eyes due to buildup of bilirubin.
- Swelling: Fluid buildup in legs, ankles, or abdomen (ascites).
- Easy bruising and bleeding: Reduced production of clotting proteins.
- Confusion and memory problems: Toxins affect the brain (hepatic encephalopathy).
- Spider angiomas: Small, red, spider-like blood vessels on skin.
- Dark urine and pale stools: Changes caused by bile flow problems.
These symptoms show the liver is severely damaged. Blood flow issues can cause pressure to build up in the portal vein, leading to serious effects.
| Symptom | Cause | Effect |
|---|---|---|
| Jaundice | Bilirubin buildup | Yellow skin and eyes |
| Swelling (Ascites) | Fluid accumulation | Abdominal discomfort |
| Easy bruising | Low clotting factors | Bleeding risk |
| Confusion | Toxin buildup in brain | Memory and thinking problems |
| Spider angiomas | Blood vessel changes | Skin appearance changes |
Complications
Cirrhosis can lead to serious health problems that affect many parts of the body. Common complications include:
- Portal Hypertension: High blood pressure in the portal vein causes varices (swollen veins) in the esophagus or stomach. These veins can bleed and be life-threatening.
- Hepatic Encephalopathy: Toxins build up and affect brain function, causing confusion, drowsiness, or coma.
- Infections: The immune system weakens, increasing risk of infections like spontaneous bacterial peritonitis.
- Liver Cancer: Cirrhosis increases the chance of developing liver cancer (hepatocellular carcinoma).
- Kidney Failure: Kidney function can decline due to liver problems, leading to hepatorenal syndrome.
Managing complications requires medical care and sometimes urgent treatment. Early detection of these problems can save lives and improve well-being.
| Complication | Description | Risk |
|---|---|---|
| Portal Hypertension | High blood pressure in liver veins | Variceal bleeding |
| Hepatic Encephalopathy | Brain toxin buildup | Confusion to coma |
| Infections | Weakened immunity | Severe infections |
| Liver Cancer | Malignant growth in liver | Life-threatening |
| Kidney Failure | Loss of kidney function | Organ failure |
Diagnosis Methods
Diagnosing cirrhosis of the liver requires a combination of methods to get a clear picture of liver health. Doctors use various tests to check liver damage and function. Early diagnosis helps manage symptoms and slow disease progression. The main diagnosis methods include physical exams, blood tests, imaging techniques, and sometimes a liver biopsy. Each method offers unique insights and helps guide treatment.
Physical Examination
A physical examination is the first step in diagnosing cirrhosis. The doctor checks for visible signs of liver problems. These signs include:
- Yellowing of the skin and eyes (jaundice)
- Swelling in the legs and abdomen
- Enlarged liver or spleen
- Spider-like blood vessels on the skin
- Red palms
The doctor also asks about symptoms like fatigue, itching, and weight loss. They check for fluid buildup in the abdomen (ascites) by pressing on the belly. The skin may be examined for bruises or bleeding, which can happen due to liver problems. Physical exams help spot signs early, but they cannot confirm cirrhosis alone.
| Physical Sign | Possible Cause |
|---|---|
| Jaundice | Build-up of bilirubin from poor liver function |
| Ascites | Fluid accumulation due to liver pressure changes |
| Spider Angiomas | Blood vessel abnormalities linked to cirrhosis |
Blood Tests
Blood tests are key to assessing liver health and function. These tests measure enzymes, proteins, and substances linked to liver damage. Common blood tests for cirrhosis include:
- Liver enzyme tests (ALT, AST): High levels indicate liver cell injury.
- Albumin: Low levels suggest poor liver protein production.
- Prothrombin time (PT): Longer clotting time shows liver dysfunction.
- Bilirubin: High amounts cause jaundice.
- Platelet count: Low count may indicate spleen enlargement due to cirrhosis.
Doctors may also check viral hepatitis markers and autoimmune antibodies to find the cause of liver damage. Blood tests do not show the liver’s structure but give important clues about how well the liver is working.
| Test | What It Shows | Normal Range |
|---|---|---|
| ALT (Alanine Aminotransferase) | Liver cell injury | 7-56 units per liter |
| AST (Aspartate Aminotransferase) | Liver damage | 10-40 units per liter |
| Albumin | Protein production by liver | 3.5-5.0 g/dL |
| Bilirubin | Liver clearance function | 0.1-1.2 mg/dL |
Imaging Techniques
Imaging tests help visualize the liver’s size, shape, and texture. These methods detect scarring, nodules, and complications of cirrhosis. Common imaging techniques include:
- Ultrasound: A simple, painless test using sound waves. It shows liver shape and fluid buildup.
- CT Scan: Provides detailed cross-sectional images of the liver and nearby organs.
- MRI: Offers high-resolution images of liver tissue and blood vessels.
- Elastography: Measures liver stiffness to assess fibrosis level.
Ultrasound is often the first choice. Elastography is a newer technique that helps track liver scarring without surgery. Imaging tests do not replace blood tests but complement them for a full diagnosis.
Liver Biopsy
A liver biopsy is the most accurate way to confirm cirrhosis. It involves removing a small liver tissue sample using a thin needle. The sample is examined under a microscope to check for:
- Extent of fibrosis or scarring
- Type of liver damage
- Presence of inflammation or fat
The biopsy helps determine the disease stage and guides treatment decisions. The procedure carries some risks, such as bleeding or pain, but complications are rare. Doctors recommend a biopsy when other tests do not give clear answers or if they need to find the exact cause of liver damage.
Before a biopsy, blood tests check for clotting ability. After the procedure, patients rest and are monitored to avoid problems. Liver biopsy remains the gold standard for diagnosing and staging cirrhosis.

Credit: www.pacehospital.com
Treatment Options
Treatment options for cirrhosis of the liver focus on slowing disease progression and managing symptoms. Early diagnosis and proper care improve quality of life. Treatment varies based on cirrhosis severity and underlying causes. Doctors combine different approaches to control liver damage and prevent complications. Patients can take active steps through lifestyle changes, medications, and medical procedures. Understanding these options helps patients make informed decisions and work with healthcare providers effectively.
Lifestyle Changes
Making lifestyle changes is a key part of managing cirrhosis. These changes help reduce liver stress and improve overall health.
- Stop Alcohol Consumption: Alcohol worsens liver damage and should be avoided completely.
- Healthy Diet: Eating balanced meals with low salt helps reduce fluid buildup.
- Maintain a Healthy Weight: Excess weight can increase liver fat and damage.
- Exercise Regularly: Light to moderate exercise improves liver function and overall wellness.
- Avoid Toxins: Limit exposure to chemicals and drugs that strain the liver.
Here is a simple table showing beneficial and harmful foods for cirrhosis patients:
| Beneficial Foods | Harmful Foods |
|---|---|
| Fresh fruits and vegetables | Processed and salty foods |
| Whole grains | Fried and fatty foods |
| Lean proteins (chicken, fish) | Alcohol and sugary drinks |
Regular checkups and following medical advice enhance the benefits of these lifestyle habits.
Medications
Medications help control symptoms and reduce complications of cirrhosis. Doctors prescribe drugs based on the patient’s condition.
- Diuretics: Reduce swelling by helping the body remove excess fluid.
- Beta-blockers: Lower blood pressure in the liver to prevent bleeding.
- Antibiotics: Treat infections common in cirrhosis patients.
- Lactulose: Helps remove toxins from the blood to improve brain function.
Medication use requires monitoring for side effects and dosage adjustments. Patients should never stop or change medicines without doctor approval.
Below is a brief overview of common medications used in cirrhosis:
| Medication | Purpose | Notes |
|---|---|---|
| Spironolactone | Diuretic to reduce fluid buildup | Monitor potassium levels |
| Propranolol | Reduce portal hypertension | Check heart rate regularly |
| Lactulose | Clear toxins from blood | May cause diarrhea |
Managing Complications
Cirrhosis can cause serious complications that need special care. Managing these problems reduces risks and improves life quality.
Common complications and their management include:
- Ascites: Fluid buildup in the abdomen managed by diuretics and salt restriction.
- Variceal Bleeding: Emergency treatment with banding or medications to stop bleeding veins.
- Hepatic Encephalopathy: Brain function improves with lactulose and infection control.
- Infections: Quick antibiotic treatment is essential to prevent worsening.
Regular monitoring helps detect complications early. Patients should report symptoms like confusion, bleeding, or swelling immediately.
Doctors may use procedures such as paracentesis to remove excess fluid or endoscopy to treat bleeding veins.
Liver Transplant
Liver transplant is a treatment option for advanced cirrhosis. It offers a chance for a new, healthy liver.
Patients with severe liver failure or life-threatening complications may be candidates for transplant. Evaluation includes:
- Overall health assessment
- Matching donor availability
- Psychological readiness
- Ability to follow post-surgery care
The transplant process involves:
- Waiting for a suitable donor liver
- Undergoing surgery to replace the damaged liver
- Taking immunosuppressant drugs to prevent organ rejection
- Regular follow-up visits and tests
Liver transplant greatly improves survival rates but carries risks like infection and rejection. Success depends on careful patient selection and medical care.
Prevention Strategies
Preventing cirrhosis of the liver is crucial to maintain liver health and avoid serious complications. Cirrhosis happens when healthy liver tissue is replaced by scar tissue, affecting its ability to work properly. Prevention strategies focus on protecting the liver from damage and supporting its natural functions. Simple lifestyle changes and regular health care can reduce the risk of cirrhosis significantly. Below are key prevention methods that help keep the liver strong and healthy.
Healthy Diet
A balanced, healthy diet supports liver function and helps prevent cirrhosis. Eating the right foods reduces the burden on the liver and lowers inflammation. Focus on:
- Fruits and vegetables: Rich in antioxidants, they protect liver cells from damage.
- Whole grains: Provide fiber, which aids digestion and reduces fat buildup in the liver.
- Lean proteins: Help repair liver tissue without adding excess fat.
- Healthy fats: Found in nuts, seeds, and fish, these fats support liver health.
Avoid processed foods high in sugar, salt, and unhealthy fats. These can increase liver stress and promote fat accumulation. Limit intake of fried foods, sugary drinks, and excessive salt.
| Good Foods for Liver | Foods to Avoid |
|---|---|
| Leafy greens (spinach, kale) | Fried and fast foods |
| Berries (blueberries, strawberries) | Sugary sodas and snacks |
| Whole grains (brown rice, oats) | Processed meats (sausages, bacon) |
| Fatty fish (salmon, mackerel) | High-salt foods |
Drinking plenty of water also helps the liver flush out toxins. Small, frequent meals can improve digestion and reduce liver workload. A healthy diet strengthens the liver’s ability to heal itself and prevents damage that leads to cirrhosis.
Limiting Alcohol
Alcohol is a major cause of liver damage and cirrhosis. The liver breaks down alcohol, but excessive drinking overworks it. This leads to inflammation, fat buildup, and scarring. To protect the liver, limit alcohol intake or avoid it completely.
Even moderate drinking can harm the liver in some people. The risk depends on factors like age, sex, and overall health. Women and older adults are more vulnerable to alcohol’s effects.
- Recommended limits: No more than one drink per day for women and two for men.
- Choose alcohol-free days: Give your liver time to recover each week.
- Avoid binge drinking: Large amounts of alcohol in a short time cause serious liver stress.
Signs of alcohol-related liver damage include fatigue, jaundice, and swelling. If these appear, stop drinking and seek medical advice immediately.
Support is available for those struggling with alcohol use. Counseling and support groups can help reduce consumption and protect liver health.
Vaccinations
Vaccinations play a key role in preventing liver infections that cause cirrhosis. Hepatitis B and Hepatitis A viruses are common causes of liver damage worldwide. Protecting against these infections lowers the chance of developing cirrhosis.
Hepatitis B spreads through blood and body fluids. Hepatitis A usually spreads by contaminated food or water. Vaccines are safe and effective in preventing these diseases.
- Hepatitis B vaccine: Recommended for all infants, unvaccinated adults, and people at higher risk.
- Hepatitis A vaccine: Suggested for travelers to certain countries and people with chronic liver disease.
Besides vaccination, practicing good hygiene reduces infection risks:
- Wash hands thoroughly before eating or preparing food.
- Avoid sharing needles or personal items like razors and toothbrushes.
- Use protection during sexual activity.
Regularly updating vaccinations and following these precautions help prevent viral hepatitis and protect liver health.
Regular Medical Checkups
Regular medical checkups help detect liver problems early before cirrhosis develops. Early diagnosis improves treatment success and prevents further liver damage.
Doctors perform tests such as:
- Blood tests to check liver enzymes and function.
- Ultrasound scans to view liver structure.
- Fibrosis tests to measure liver scarring.
People with risk factors like viral hepatitis, heavy alcohol use, or obesity need frequent monitoring. Checkups allow doctors to:
- Identify liver disease early.
- Advise lifestyle or medication changes.
- Track disease progression and adjust treatment.
Early detection also helps prevent complications such as liver failure or cancer. Don’t wait for symptoms to appear. Schedule regular visits and follow your doctor’s advice to protect your liver.
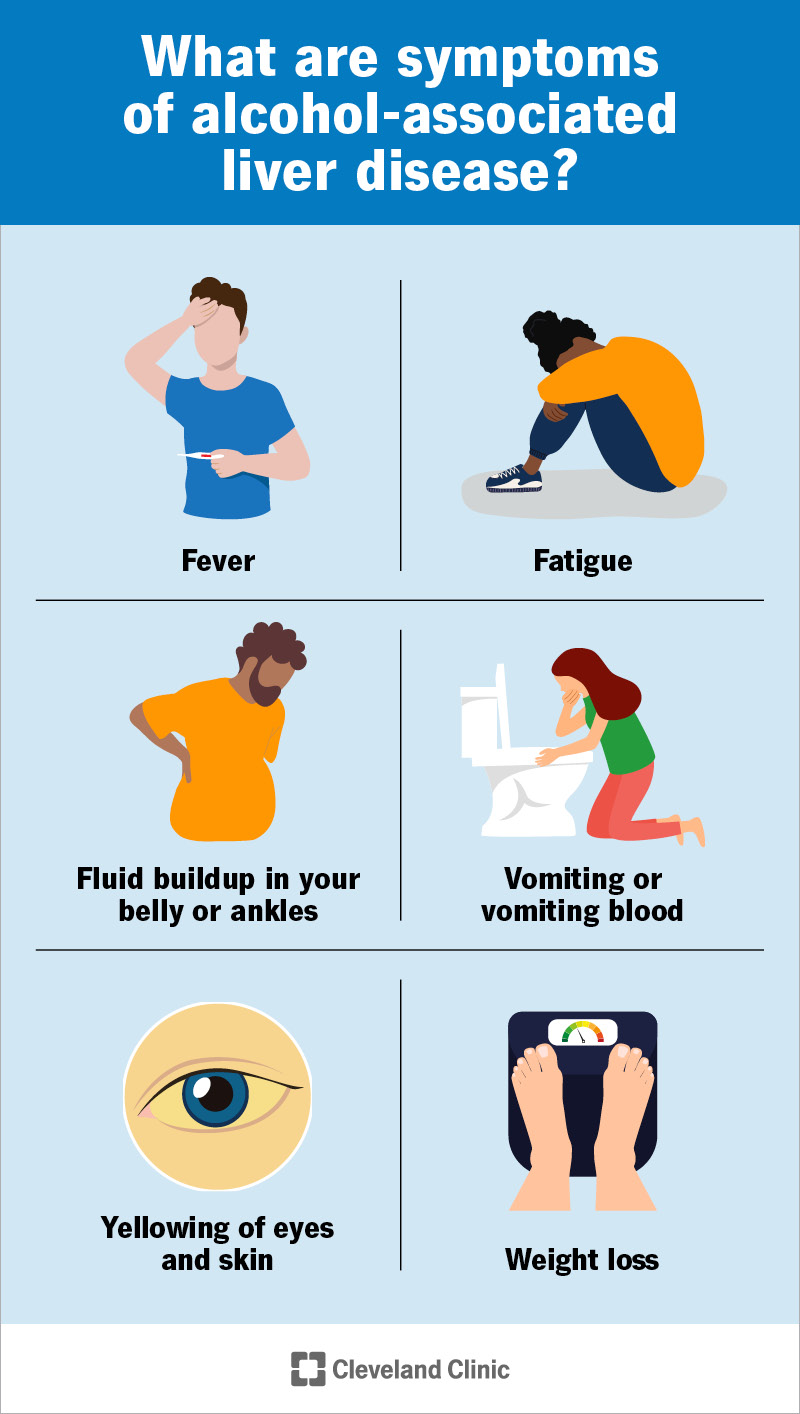
Credit: my.clevelandclinic.org
Frequently Asked Questions
What Causes Cirrhosis Of The Liver?
Cirrhosis is mainly caused by chronic liver damage from alcohol abuse, hepatitis B or C, and fatty liver disease. These conditions lead to scarring and impaired liver function over time.
What Are Common Symptoms Of Liver Cirrhosis?
Symptoms include fatigue, jaundice, swelling in legs, abdominal pain, and easy bruising. Early signs are often mild, but worsen as scarring progresses.
How Is Cirrhosis Diagnosed By Doctors?
Doctors diagnose cirrhosis through blood tests, imaging like ultrasound, and sometimes a liver biopsy. These help assess liver damage and function.
Can Cirrhosis Be Treated Or Reversed?
While cirrhosis damage is mostly irreversible, treatment can slow progression. Managing underlying causes and lifestyle changes improve quality of life.
Conclusion
Cirrhosis of the liver is a serious condition that needs attention. Early signs can be mild but should not be ignored. Recognizing symptoms helps in seeking timely treatment. Treatment can slow damage and improve life quality. Healthy habits support liver health and recovery.
Regular check-ups help catch problems early. Stay informed and talk to your doctor about concerns. Taking care of your liver is important for your overall well-being.