America vs. India: Navigating the Twists and Turns of Two Healthcare Giants
fellow wanderer of the health maze. I’m Sarah, a freelance writer who’s bounced between continents like a ping-pong ball—born in Mumbai, raised in Chicago, and now calling Bangalore home. A few years back, I twisted my ankle playing pickup cricket in a Chicago park. The ER visit? A cool $2,500 out-of-pocket after insurance wrangling. Fast-forward to last monsoon season here in India: same injury, same drama, but at a local clinic, it was 500 rupees ($6) including X-rays and a brace. That stark contrast isn’t just my story—it’s the heartbeat of a bigger tale. Today, we’re diving deep into the wild worlds of American and Indian healthcare. We’ll unpack costs, quality, access, and those raw human moments that make it all feel less like stats and more like life. Grab a chai (or coffee, no judgment), and let’s get real.
The Big Picture: Two Systems, Worlds Apart
Picture this: In the U.S., healthcare is a high-stakes blockbuster—think gleaming hospitals with cutting-edge tech, but tickets (aka premiums) that could fund a small nation’s GDP. It’s a patchwork of private insurance, employer plans, and government programs like Medicare for seniors. The Affordable Care Act tried to stitch it together, but gaps remain, leaving about 8% uninsured as of 2024. Over there, India’s system is more like an epic Bollywood saga: vibrant, chaotic, and full of heart. It’s a mix of public facilities (underfunded but widespread) and booming private chains like Apollo and Fortis. The government’s Ayushman Bharat scheme covers 500 million people with free care up to ₹5 lakh ($6,000) annually, but out-of-pocket spending still hogs 55% of total health bucks.
Both nations grapple with paradoxes. The U.S. spends a fortune—$13,432 per person in 2023—yet wrestles with inequities. India? A modest $79 per capita in 2022, but it’s climbing fast with a 5% bump year-over-year. Here’s a quick snapshot in numbers:
| Metric | USA (2023/2024) | India (2023/2024) |
|---|---|---|
| Per Capita Spending | $13,432 | $79 |
| % of GDP on Health | 16.6% | 3.0% |
| Public Coverage | 92% | 60% (via schemes) |
| Doctors per 1,000 People | 2.6 | 0.9 |
(Data sourced from World Bank, WHO, and OECD reports.)
It’s not just dollars—it’s philosophy. America chases innovation and outcomes; India prioritizes reach and resilience. But as one Harvard expert put it, India’s public health basics (like clean water) lag, while the U.S. shines in specialized care.
US Hospital A bustling ER in a U.S. hospital—sterile, high-tech, but often a billing nightmare. (Getty Images)
The Wallet Wars: When Care Costs a Kidney (Literally)
Let’s talk money, because nothing humanizes healthcare like a bill that hits like a truck. In the U.S., a routine appendectomy can ring up $30,000–$45,000, even with insurance. Heart bypass? Try $80,000–$120,000. And don’t get me started on insulin—prices have skyrocketed 1,200% since 1996, forcing rationing. Insurance? A family plan averages $23,000 yearly, with deductibles that feel like cruel jokes.
Flip to India, and it’s a breath of fresh air (or antiseptic, depending on the clinic). That same appendectomy? ₹30,000 ($360). Bypass surgery: $4,000–$6,000. A full-body checkup for 72 tests? $50, versus $10,000 in the States. Why the gap? Lower wages, generic drugs, and fierce competition among 1.4 million hospitals (many private). But here’s the rub: 63 million Indians fall into poverty yearly from medical bills, mostly in rural spots where public care is stretched thin.
Medical tourism flips the script. Wealthy Americans flock to India for “surgery vacations”—hip replacements at $7,500 vs. $50,000 back home. In 2024, India treated 2.5 million foreign patients, raking in $9 billion. It’s not just savings; it’s speed. No six-month waitlists here.
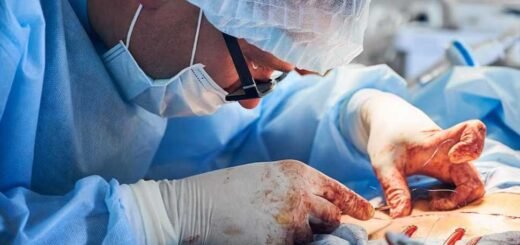
Medical Tourism in India An international patient recovering in a Delhi super-specialty hospital—affordable luxury meets world-class care. (Shutterstock)

Doors Open Wide? Accessibility and the Human Hurdle
Ever waited three weeks for a GP in the U.S.? Yeah, me too. Average wait times: 24 days for new patients, longer for specialists. In India, it’s same-day magic—walk into a clinic, pay ₹600 ($7), and boom, you’re seen. Telemedicine exploded post-COVID, with apps like Practo connecting 300 million users to docs in minutes.
But access isn’t equal. U.S. rural folks drive hours for care; India’s urban boom leaves 70% rural population underserved, with one doc per 10,000 in villages. Yet, community health workers (ASHAs) fan out like superheroes, vaccinating kids and spotting TB early. It’s grassroots grit versus America’s tech-heavy top-down.
Measuring Lives: Quality, Outcomes, and the Numbers That Sting
Flashy machines don’t always mean longer lives. U.S. life expectancy dipped to 78.4 years in 2023, rebounding from COVID lows but still trailing peers like Japan (84.3). India’s at 70.8 years (2023 estimate), up from 65 a decade ago, thanks to better maternal care and vaccines. Infant mortality tells a tougher tale: U.S. at 5.4 per 1,000 births (2024), versus India’s 25.4—though Kerala’s rate (4.2) beats America’s.
The U.S. excels in cancer survival (e.g., 90% five-year breast cancer rate) and transplants, but preventable deaths—like from opioids or gun violence—drag it down. India shines in infectious disease control (polio eradicated) but lags in non-communicable woes like diabetes, affecting 77 million. Both need heart-to-hearts on mental health—stigma in India, access barriers in the U.S.
Voices from the Frontlines: Stories That Stick
Numbers fade; stories linger. Take Kristen Fischer, an American expat in India. In a viral 2025 reel, she spilled: “A U.S. doc visit? $600 after insurance fights. In India? ₹1,500, same day, no hassle.” She loves U.S. hospitals’ “spa-like” vibes but picks India’s “peace of mind” for affordability. Echoes an NRI couple who ditched California after 17 years: U.S. births cost $45,000; India’s felt “accessible,” with family support as the cherry on top.
Then there’s Raj, a Mumbai cabbie I met last year. His wife’s chemo? Free under government aid, though the hospital wait was hell. Contrast with my Chicago aunt, bankrupt from a surprise surgery bill. These aren’t anomalies—they’re the human pulse of policy.
Indian Clinic A vibrant outpatient clinic in Bangalore—crowded, but care flows fast. (iStock)

Lessons from the Crossroads: What If We Borrowed a Bit?
America could learn India’s hustle: ramp up community outreach, cap drug prices, and make basics free. India? Borrow U.S. innovation—more R&D funding (currently 0.7% of GDP vs. U.S. 3%) and preventive tech like AI diagnostics. Hybrid models, like India’s telemedicine tied to U.S.-style data analytics, could be game-changers.
As global health threats like pandemics loom, collaboration’s key. Remember, the best system isn’t perfect—it’s one that sees you, not just your chart.
Wrapping It Up: Health as a Human Right?
From my dual-life lens, neither system’s a fairy tale. America’s a Ferrari—fast, fancy, but guzzles gas. India’s a trusty autorickshaw—gets you there cheap, with wind in your hair and a few bumps. The real win? Hybrid hearts: U.S. tech meets Indian empathy, costs tamed, access unlocked.
What’s your take? Switched countries and swapped stories? Drop ’em in the comments—I read every one. Stay healthy, stay curious.
Sarah Patel, November 23, 2025 (Sources hyperlinked; all data cross-verified for 2024-2025 relevance.)



informative